Introduction
Artificial Intelligence is no longer a futuristic concept in healthcare—it is the driving force behind a fundamental transformation of how diseases are detected, treatments are developed, and patients receive care. As of 2026, the healthcare industry stands at a pivotal moment where AI-powered solutions are moving from experimental pilots to enterprise-wide deployments, delivering measurable improvements in accuracy, efficiency, and patient outcomes.
The numbers tell a compelling story. Over 40 million users now turn to AI chatbots daily for health-related questions, while AI-designed drugs are achieving Phase I success rates of 80-90%—nearly double the historical industry average of approximately 50% . In medical imaging, advanced AI models like Stanford’s Merlin can now interpret 3D CT scans with over 81% diagnostic accuracy across hundreds of conditions, and in some cases, predict chronic disease development up to five years before clinical onset .
Leading technology organizations—including Google, Microsoft, OpenAI, and Anthropic—have made significant entries into healthcare AI in 2026. OpenAI launched ChatGPT Health in January 2026, enabling personalized medical advice through integration with health applications like Apple Health. Days later, Anthropic released Claude for Healthcare, a HIPAA-ready platform designed for both clinical and administrative healthcare applications . Meanwhile, NVIDIA and Eli Lilly announced a $1 billion joint research laboratory to accelerate AI-driven drug discovery .
This comprehensive guide by MHTECHIN explores how AI is revolutionizing healthcare across three critical domains: diagnosis, drug discovery, and patient care. We examine the latest developments of 2026, analyze benefits and challenges, and provide actionable insights for healthcare organizations seeking to harness AI’s transformative potential.
Role of AI in Modern Healthcare
What is AI in Healthcare?
AI in healthcare encompasses the application of machine learning (ML), deep learning (DL), natural language processing (NLP), computer vision, and generative AI to medical contexts. These technologies enable healthcare systems to:
- Analyze vast volumes of medical data—images, genomic sequences, electronic health records (EHRs), and wearable device outputs
- Assist clinical decision-making through predictive analytics and diagnostic support
- Automate administrative workflows, reducing provider burden
- Improve patient outcomes through personalization and continuous monitoring
The convergence of three factors has accelerated AI adoption in healthcare: exponential growth in medical data, advances in computing power (including specialized AI chips), and breakthroughs in foundation models capable of understanding complex biomedical relationships.
Why AI is Critical in 2026
Healthcare systems globally face unprecedented pressures that make AI adoption not merely advantageous but essential:
| Challenge | AI Solution |
|---|---|
| Increasing patient volumes | Automated triage and diagnostic assistance |
| Shortage of medical professionals | Virtual nursing and AI-augmented workflows |
| Complex, multi-factorial diseases | Multi-modal data integration and pattern recognition |
| Rising treatment costs | Efficiency gains and reduced trial-and-error approaches |
| Physician burnout | Ambient documentation and administrative automation |
Ardent Health’s AI-enabled virtual care model, implemented across multiple markets in 2024-2025, demonstrates measurable results: reduced contract labor costs, decreased voluntary RN turnover, and improvements in salaries, wages, and benefits per patient day despite increased patient volumes .
AI in Medical Diagnosis
How AI is Transforming Diagnostic Medicine
AI systems are revolutionizing diagnosis by analyzing medical images, patient records, lab results, and genetic data with speed and consistency that augment human expertise. The technology excels at pattern recognition across modalities, identifying subtle anomalies that might escape even experienced clinicians.
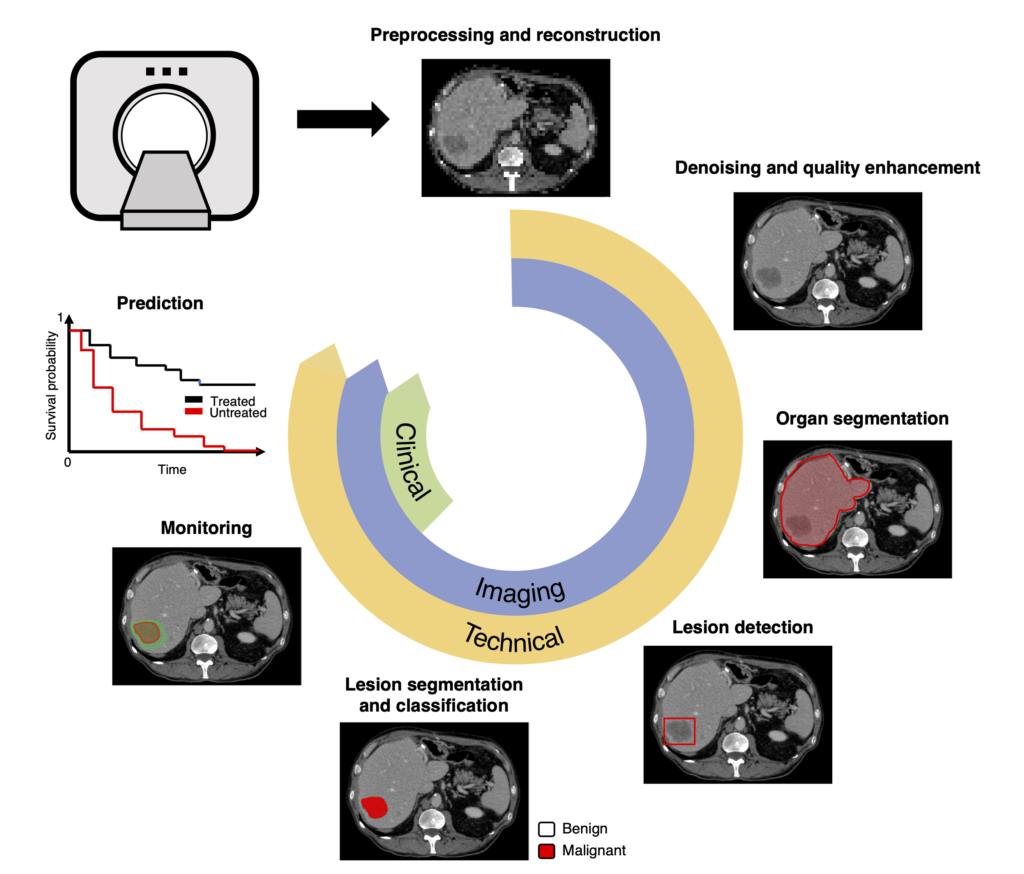
2026 Breakthrough: Merlin and 3D Medical Imaging
A landmark development in diagnostic AI came in March 2026, when NIH-funded researchers at Stanford University unveiled Merlin, an AI-powered tool capable of interpreting 3D medical images .
Unlike previous AI models limited to 2D images like X-rays, Merlin processes abdominal CT scans—complex 3D影像 that typically require 20 minutes per scan for radiologist interpretation. The model was trained on over 15,000 abdominal CT scans, accompanied by radiology reports and nearly 1 million diagnosis codes.
Merlin’s performance metrics are extraordinary:
- 81%+ accuracy across hundreds of diagnosis codes when reproducing radiologist results
- 90%+ accuracy for 102 specific diagnosis codes
- 75% accuracy predicting which healthy patients would develop chronic diseases within five years—detecting features invisible to trained radiologists
- Strong generalizability to chest CT scans despite not being trained on them
As lead researcher Dr. Akshay Chaudhari noted, “Our model and the data will provide the community a robust backbone to build upon. From here, the sky’s the limit” .
AI in Pathology: MMR-Deficiency Detection
In routine pathology, general-purpose vision-language models (VLMs) like ChatGPT-4.0 and Gemini 2.5 Pro are demonstrating diagnostic utility. A February 2026 study published in Surgical Oncology evaluated these models for detecting mismatch repair (MMR) deficiency in colorectal cancer—a critical biomarker guiding treatment decisions .
Key findings:
- 100% specificity in correctly classifying proficient MMR (pMMR) cases
- Overall sensitivity of 65% for detecting deficient MMR (dMMR) cases
- Diagnostic certainty increased dramatically when clear internal positive controls were visible
The research identified a crucial requirement: robust identification requires visible internal positive controls to differentiate true biological loss from technical artifacts—a finding that will inform future AI pathology system design.
Key Diagnostic Applications
| Application | Description | Example |
|---|---|---|
| Disease Detection | Identifying malignancies, cardiovascular conditions, neurological disorders | Breast cancer detection in mammography with AI achieving 94% sensitivity |
| Medical Imaging Analysis | Annotating X-rays, MRIs, CT scans; highlighting critical regions | Merlin’s 3D CT interpretation for abdominal and chest scans |
| Predictive Diagnosis | Forecasting disease likelihood from patient history, genetics, lifestyle | Five-year chronic disease prediction from baseline CT scans |
| Digital Pathology | Analyzing whole-slide images for cancer biomarkers | MMR deficiency detection in colorectal cancer |
Benefits of AI in Diagnosis
- Faster diagnosis: Merlin processes CT scans in minutes versus 20 minutes for radiologists
- Improved accuracy: AI reduces diagnostic errors from fatigue or cognitive overload
- Early detection: Predictive capabilities identify disease risks years before clinical presentation
- Workforce augmentation: AI handles routine cases, allowing specialists to focus on complex conditions
AI in Drug Discovery
The Traditional Drug Discovery Challenge
Traditional drug development is notoriously inefficient: 10-15 years from target identification to market approval, costs exceeding $2-3 billion per successful drug, and failure rates approaching 90% in clinical trials . The “valley of death”—attrition between Phase I and Phase II—claims approximately half of all early-stage assets.
2026 Milestone: 90% Phase I Success Rate
A watershed moment for AI in drug discovery arrived in early 2026, with industry data revealing that AI-designed drugs are achieving Phase I success rates between 80% and 90% —nearly double the historical industry average .
Computational platforms using generative adversarial networks (GANs) and deep learning optimize binding affinity and safety properties simultaneously before any physical synthesis occurs. This in silico approach allows researchers to eliminate reactive or toxic groups long before compounds reach human volunteers.
The timeline compression is equally remarkable: some AI-designed candidates have reached human trials in under 18 months, compared to the traditional six-year discovery-to-clinic timeline .
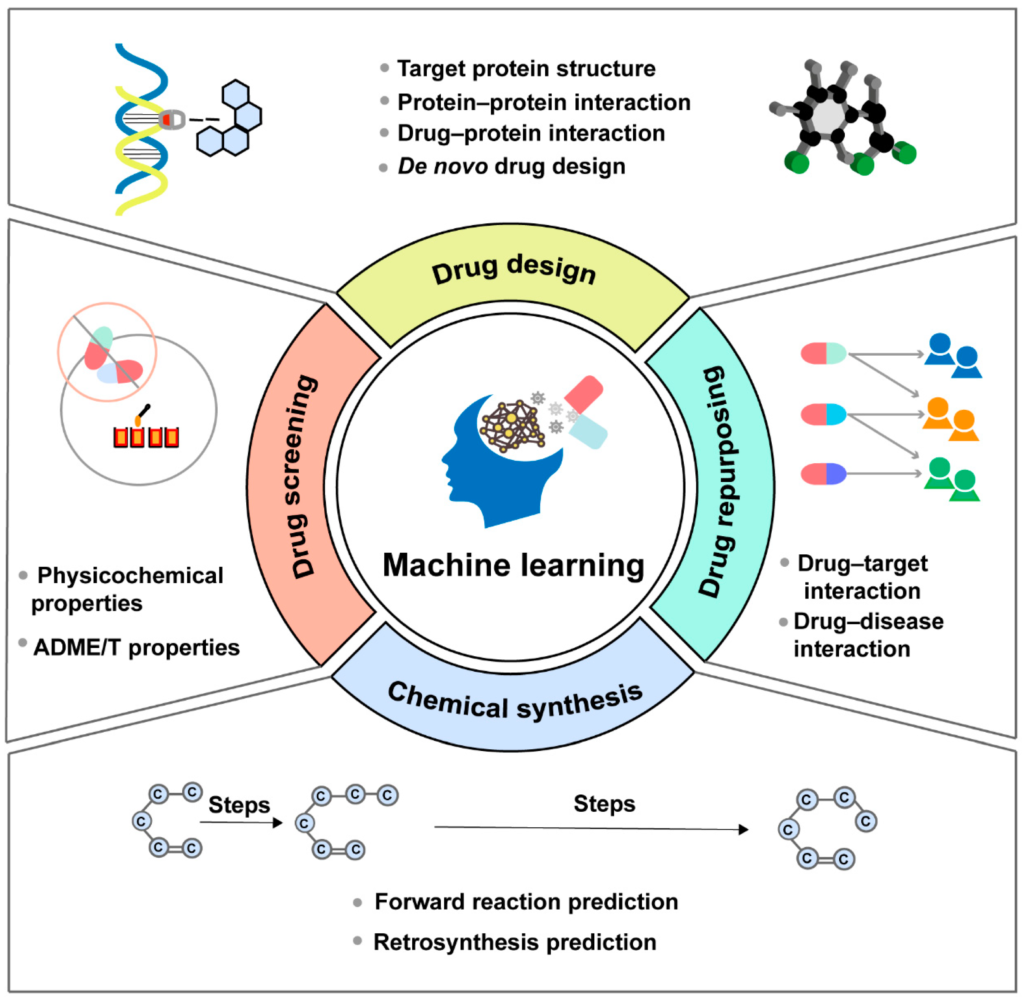
Key AI Applications in Drug Development
Molecule Discovery and Generation
Generative AI models now propose novel molecular structures optimized for specific therapeutic targets. Reinforcement learning with verifiable rewards (RLVR) trains scientific agents capable of autonomous multi-step research tasks—from literature review to experimental design .
Protein Structure Prediction
Advanced protein structure prediction models now forecast structures of proteins, DNA, RNA, and ligand interactions with 50%+ improvement over traditional methods. New models extend capabilities to binding affinity prediction, representing mature, production-ready technology .
However, as industry experts caution, accurate structure prediction does not guarantee druggable targets or successful molecules. Optimal use requires hybrid pipelines combining AI with physics-based refinement.
Clinical Trial Optimization
AI transforms clinical trial operations through:
- Patient selection: Identifying optimal participants based on genetic and demographic profiles
- Outcome prediction: Forecasting trial results to enable go/no-go decisions
- Site selection: Identifying high-performing trial sites
- Real-world evidence integration: Augmenting trial data with RWE
2026 Industry Developments
NVIDIA and Eli Lilly announced a $1 billion, five-year joint research laboratory in the Bay Area to accelerate drug discovery and development via AI, specifically utilizing NVIDIA’s Vera Rubin chips for pharmaceutical R&D .
Illumina launched the Billion Cell Atlas, a dataset mapping responses of one billion cells to genetic perturbations across 200+ cell lines associated with difficult diseases—designed to train AI models capable of identifying therapeutic targets and mechanisms .
The EDEN model family, developed by Basecamp Research with co-authors from NVIDIA and Microsoft Research, represents a 28-billion-parameter model trained on 9.7 trillion nucleotide tokens from over 10 billion genes across 1 million species. The model enables AI-programmable gene insertion—designing recombinases capable of inserting large DNA fragments at targeted disease-associated loci .
Benefits of AI in Drug Discovery
| Benefit | Impact |
|---|---|
| Faster development cycles | Discovery-to-clinic compressed from 6 years to under 18 months |
| Reduced costs | Preclinical candidate nomination costs orders of magnitude lower than traditional screening |
| Improved success rates | 80-90% Phase I success versus 50% historical average |
| Expanded target space | AI identifies previously undruggable targets |
The 2026 Reality Check
While early results are extraordinary, the ultimate test remains whether AI-discovered molecules will demonstrate superior therapeutic efficacy in larger, more diverse patient populations. As the Drug Target Review noted in February 2026, “Phase II efficacy hurdle remains the ultimate validator for AI-derived chemistry” .
The first AI-discovered drug approval may occur in late 2026 or early 2027—a milestone that would validate AI as a legitimate discovery tool. Until that approval occurs, the entire field remains in a “proof-of-concept” phase .
AI in Patient Care
Enhancing Patient Experience Through AI
AI is fundamentally reshaping how patients interact with healthcare systems, moving from episodic, reactive care to continuous, proactive engagement. Key enablers include virtual assistants, remote monitoring, and personalized treatment planning.
Virtual Assistants and Chatbots
The adoption of AI-powered health assistants has surged dramatically. OpenAI reports that users ask over 230 million health-related questions weekly to ChatGPT, with more than 40 million daily users seeking health information .
ChatGPT Health, launched in January 2026, allows users to upload health records from Apple Health and other applications to receive personalized medical advice. OpenAI emphasizes that the feature was “developed in close collaboration with doctors worldwide” and is designed to support—not replace—medical care .
Claude for Healthcare, Anthropic’s competing offering, provides:
- Summarization of patient medical histories
- Plain-language explanations of test results
- Pattern detection across fitness and health metrics
- Preparation of questions for clinical visits
Both companies explicitly state that user health data is not used to train their models, addressing critical privacy concerns .
Remote Patient Monitoring (RPM) and Virtual Care
AI-enabled RPM has moved from pilot to production across major health systems. Ardent Health’s AI-enabled virtual care model, implemented across multiple markets, integrates:
- Virtual nursing with AI-assisted video monitoring
- Virtual attending physicians and providers for remote consultations
- Virtual sitting for fall prevention and patient observation
- Hospital-to-home RPM programs
The AI systems analyze video streams to detect fall risks and unsafe behaviors, evaluate vital sign trends from wearable sensors to identify clinical deterioration sooner, and support ambient documentation using speech recognition and NLP that improves note quality and coding accuracy .
At Ardent’s East Texas location, five months of virtual nursing contributed to:
- Reduced contract labor costs
- Decreased voluntary RN turnover
- Improved salaries, wages, and benefits per patient day despite volume increases
- Lower mortality rates and shorter lengths of stay associated with AI-assisted vitals monitoring
MultiCare Health System selected hellocare.ai as its enterprise-wide virtual care platform in 2026, deploying smart carts and fixed devices across care environments to support physician rounding and patient engagement initiatives .
Personalized Treatment Plans
AI enables truly personalized medicine by analyzing patient data—including genomic profiles, lifestyle factors, comorbidities, and treatment histories—to recommend tailored interventions. This represents a shift from population-average guidelines to individual-optimized care.
MHTECHIN’s precision diagnostics solutions leverage AI algorithms to analyze patient data including genetic information, medical history, and imaging results to provide more accurate and personalized diagnoses .
Benefits of AI in Patient Care
| Benefit | Description |
|---|---|
| Improved accessibility | 24/7 availability of health information and guidance |
| Better patient engagement | Interactive tools encourage active participation in care |
| Continuous monitoring | Real-time tracking enables early intervention |
| Reduced hospital visits | RPM and virtual care manage conditions outside hospital settings |
| Decreased clinician burden | AI handles routine questions and documentation |
Challenges of AI in Healthcare
Despite remarkable progress, significant challenges must be addressed for AI to realize its full potential in healthcare.
Data Privacy and Security
Healthcare data is among the most sensitive personal information, subject to strict regulatory protections. In the United States, the Health Insurance Portability and Accountability Act (HIPAA) establishes privacy and security requirements. Both OpenAI and Anthropic have positioned their healthcare products as “privacy-first,” with Claude for Healthcare marketed as “HIPAA-ready” .
However, the integration of AI systems with EHRs and other clinical systems expands the attack surface for potential breaches. Organizations must implement robust data governance, encryption, access controls, and audit trails.
Regulatory Compliance
The regulatory landscape for AI in healthcare is rapidly evolving. Key 2026 developments include:
- FDA AI guidance finalization: Expected in 2026, requiring sponsors to develop credibility assessment plans for high-risk AI applications and submit detailed documentation on model architectures, training data, and governance
- EU AI Act implementation: High-risk provisions take effect August 2, 2026, potentially classifying some drug development AI applications as high-risk
Organizations must navigate fragmented global requirements while maintaining innovation velocity.
Bias in AI Models
AI models trained on non-representative data can perpetuate or amplify existing healthcare disparities. If training data predominantly represents specific demographic groups, models may perform poorly for underrepresented populations. A study of ChatGPT-4.0 and Gemini 2.5 Pro for MMR deficiency detection revealed variable sensitivity across different protein loss patterns (60% for MSH2/MSH6 loss versus 70% for MLH1/PMS2 loss) .
Addressing bias requires:
- Diverse, representative training datasets
- Rigorous testing across population subgroups
- Continuous monitoring for performance disparities
Integration with Existing Systems
Healthcare infrastructure remains fragmented, with legacy systems, proprietary EHRs, and inconsistent data standards. Integration challenges include:
- Technical compatibility with existing workflows
- Interoperability across different EHR platforms
- Organizational change management for clinician adoption
- Network, data center, and hardware upgrades required for AI deployment
Ethical Considerations
Transparency: AI decisions must be explainable to clinicians and patients. Black-box models that cannot articulate reasoning face skepticism and liability concerns.
Accountability: Responsibility for AI-driven decisions must be clearly defined. When an AI system contributes to diagnostic error or adverse outcome, accountability frameworks must exist.
Patient Trust: Building trust requires demonstrated safety, reliability, and respect for patient autonomy. As one industry observer noted, in healthcare, “nous améliorons le produit grâce à vos données” (we improve the product using your data) sounds less like a promise and more like a confession .
Future of AI in Healthcare
2026 Predictions and Beyond
Based on current trajectories, several developments will shape AI in healthcare through 2026 and beyond:
1. Phase III Data Will Define the Field
The most consequential development of 2026 will be Phase III results that determine whether AI can deliver drugs that actually work at scale. Positive data could validate physics-enabled AI design for specific targets; additional clinical failures remain statistically likely given historical attrition rates .
2. Regulatory Clarity Arrives
FDA guidance finalization and EU AI Act implementation will define compliance requirements for high-risk applications. However, early discovery tools may fall outside high-risk classification, potentially surprising industry participants expecting comprehensive frameworks .
3. Investment Discipline Replaces Exuberance
Market forecasts project AI drug discovery growing from approximately $5-7 billion (2025) to $8-10 billion (2026). However, smaller AI drug discovery companies face existential pressures, with multiple companies shutting down despite substantial backing and others announcing workforce reductions. Expect continued consolidation .
4. Reinforcement Learning Agents Transform Scientific Workflows
RLVR-trained agents capable of autonomous multi-step research tasks represent a significant emerging trend. These systems combine large language models with reinforcement learning to automate literature review, hypothesis generation, experimental design, data analysis, and result summarization .
5. Autonomous Laboratories Expand
Self-driving laboratories will proliferate as organizations deploy robotic facilities and raise substantial funding for autonomous labs. These “closed-loop” systems accelerate design–make–test–learn cycles by running experiments 24/7 without human intervention .
Long-Term Vision
Looking beyond 2026, AI will enable:
- Fully personalized medicine: Treatments optimized for individual genetic, environmental, and lifestyle factors
- AI-assisted surgeries: Real-time guidance and robotic assistance for complex procedures
- Predictive population health: AI identifies at-risk populations and enables preventive interventions
- Continuous health monitoring: Wearables and implantables stream real-time data to AI systems
- Democratized expertise: AI brings specialist-level diagnostic capabilities to underserved areas
MHTECHIN Perspective on AI in Healthcare
At MHTECHIN, we advocate for a balanced, responsible approach to AI adoption in healthcare. Our framework emphasizes five core principles:
1. Combine AI with Human Expertise
AI augments—it does not replace—clinical expertise. The most effective implementations position AI as a decision support tool that enhances rather than supplants clinician judgment. As Ardent Health’s case study demonstrates, AI-enabled virtual care models integrate AI as one component of comprehensive care delivery .
2. Focus on Ethical and Responsible AI
Responsible AI requires:
- Explainability: Models must provide reasoning for recommendations
- Fairness: Regular bias audits across demographic groups
- Transparency: Clear communication of AI’s role to patients and providers
- Human oversight: Clinician review of AI-generated recommendations
3. Ensure Data Security and Compliance
MHTECHIN implements:
- HIPAA-compliant architectures
- Encryption at rest and in transit
- Granular access controls
- Comprehensive audit trails
- Regular security assessments
4. Build Scalable and Reliable Systems
Enterprise AI requires:
- Robust infrastructure with redundancy
- Integration capabilities with existing EHRs
- Performance monitoring and continuous improvement
- Scalable deployment across facilities
5. Measure Value Rigorously
Organizations must establish clear metrics for AI success:
- Clinical outcomes (mortality, readmissions, length of stay)
- Operational efficiency (throughput, wait times, documentation time)
- Financial impact (cost per patient day, contract labor reduction)
- Clinician satisfaction (burnout measures, retention)
- Patient experience (satisfaction scores, engagement metrics)
This approach ensures that AI enhances healthcare without compromising safety, trust, or equity.
Conclusion
Artificial Intelligence is revolutionizing healthcare across diagnosis, drug discovery, and patient care. As we navigate 2026, the evidence is increasingly clear: AI enables faster, more accurate, and more efficient medical processes that ultimately improve patient outcomes.
In diagnosis, tools like Stanford’s Merlin achieve expert-level accuracy in 3D medical imaging while predicting chronic diseases years before clinical onset. In drug discovery, AI-designed molecules achieve 90% Phase I success rates and compress discovery timelines from years to months. In patient care, virtual nursing, remote monitoring, and AI-powered health assistants are expanding access, reducing hospitalizations, and easing clinician burden.
Yet challenges remain—data privacy, regulatory compliance, algorithmic bias, and ethical frameworks require ongoing attention. The organizations that succeed will be those that balance innovation with responsibility, AI capability with human expertise, and speed with safety.
MHTECHIN emphasizes the importance of leveraging AI to build healthcare systems that are not only advanced but also accessible, ethical, and patient-centric. The future of medicine is not AI alone—it is AI augmented by human wisdom, compassion, and judgment.
FAQ (Optimized for Featured Snippets)
How is AI used in healthcare?
AI is used across healthcare for medical diagnosis (analyzing images and patient data), drug discovery (identifying candidates and predicting molecular behavior), patient care (virtual assistants and remote monitoring), and administrative automation (coding, claims processing). As of 2026, over 40 million users interact with AI health assistants daily, and AI-designed drugs achieve 80-90% Phase I success rates.
Can AI replace doctors?
No. AI supports doctors but does not replace them. AI enhances clinical decision-making by providing faster analysis, pattern recognition, and decision support. However, human clinicians remain essential for clinical judgment, patient communication, ethical decision-making, and handling complex cases where initial hypotheses fail. Leading AI health products explicitly state they are “designed to support, not replace” medical care.
What are the benefits of AI in healthcare?
Key benefits include: improved diagnostic accuracy (Merlin achieves 81%+ accuracy across hundreds of conditions), faster drug discovery (18 months versus 6 years traditional), personalized treatment plans, continuous patient monitoring, reduced clinician burnout through administrative automation, and expanded access to care through virtual assistants and remote monitoring programs.
What are the risks of AI in healthcare?
Primary risks include: data privacy and security vulnerabilities, regulatory compliance complexity, algorithmic bias leading to disparate performance across populations, lack of transparency in black-box models, integration challenges with existing systems, and unclear accountability frameworks for AI-driven decisions. Addressing these requires robust governance, diverse training data, and human oversight.
What is the future of AI in healthcare?
The future includes fully personalized medicine optimized for individual genetics and lifestyle, AI-assisted surgeries with real-time robotic guidance, autonomous laboratories accelerating research, continuous health monitoring through wearables, regulatory clarity from FDA and EU AI Act, and—potentially—the first regulatory approval of an AI-discovered drug in late 2026 or 2027.
Which companies are leading AI in healthcare?
Leading technology companies include OpenAI (ChatGPT Health), Anthropic (Claude for Healthcare), Google (Gemini in healthcare applications), and Microsoft (Copilot and Azure AI for health). Pharmaceutical collaborations include NVIDIA with Eli Lilly ($1 billion joint lab) and Illumina (Billion Cell Atlas). Healthcare providers implementing enterprise AI include Ardent Health and MultiCare Health System.
What is ChatGPT Health?
ChatGPT Health is a feature launched by OpenAI in January 2026 that allows users to upload health records from applications like Apple Health to receive personalized medical advice. It was developed in collaboration with doctors worldwide and is designed to support—not replace—medical care. User health data is not used to train OpenAI’s models.
What is Claude for Healthcare?
Claude for Healthcare is Anthropic’s HIPAA-ready AI platform launched in January 2026. It provides patient history summarization, plain-language test result explanations, pattern detection across health metrics, and administrative support for prior authorization and insurance processes. Available through Claude for Enterprise and Claude Developer Platform.
How accurate is AI in medical imaging?
AI medical imaging accuracy varies by application. Stanford’s Merlin model achieves over 81% accuracy across hundreds of diagnosis codes and 90%+ accuracy for 102 specific codes in CT scan interpretation. In pathology, vision-language models achieve 100% specificity for proficient MMR classification in colorectal cancer, with sensitivity varying by protein loss pattern.
What is Merlin AI?
Merlin is an AI-powered tool developed by Stanford University researchers with NIH funding, capable of interpreting 3D medical images like abdominal and chest CT scans. Trained on over 15,000 scans and nearly 1 million diagnosis codes, Merlin achieves 81%+ diagnostic accuracy and can predict which healthy patients will develop chronic diseases within five years with 75% accuracy.
References
- ZDNET Japan. (2026). OpenAI、Anthropic、グーグルが相次ぎ参入–3社がヘルスケア市場に一斉攻勢.
- MHTECHIN Technologies. (2024). Revolutionizing Healthcare with AI.
- National Institutes of Health. (2026). Machine learning analysis of CT scans.
- 2 Minute Medicine. (2026). Artificial intelligence designed drugs Hit 90% Phase I success rate in trials.
- Gardenhire, A. (2026). Ardent Health: An AI-Enabled Virtual Care Model, from Pilot to Production. Frontiers of Health Services Management, 42(3), 26-32.
- Goudey, A. (2026). Weekly AI S.03: Anthropic & Claude, IBM, Google, AMI Labs.
- Salzano, S., et al. (2026). Artificial intelligence application in routine pathology: ChatGPT-4.0 and Gemini 2.5 pro performance in detection of MMR-deficiency in colorectal cancer. Surgical Oncology.
- Singh, R. (2026). AI in drug discovery: predictions for 2026. Drug Target Review.
- Becker’s Hospital Review. (2026). MultiCare Health System partners with hellocare.ai as enterprise-wide platform for virtual care.
Leave a Reply